Podcast

Insight & Actions Podcast
Insight & Actions Podcast

43:23

40:14

50:12

48:01

35:36

46:02

45:07

51:03

42:44

05:48

39:30

39:01

45:30

05:46

45:12

40:30

01:15

00:59

00:42

00:41

01:11

00:48

00:48
00:48
00:50

03:02
Inside Substance Use Treatment: Real Stories, Recovery Residences, and Loneliness in Early Sobriety
Insight Recovery Centers’ executive director Chrissy Chow joins the Insights & Actions podcast to discuss the good and bad of the substance use industry and share personal stories.
Expect to hear:
- the good and bad of recovery residences
- kratom reform,
- when psychology becomes cult-ish,
- getting sober and feeling worse,
- CBT and IFS,
and more!
Tips for life transitions (when kids leave, research on happiness, and fatherhood)
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, LSATP and Johnny Pierce, PsyD discuss how to thrive when life changes.
Expect to hear:
- Tips for dealing with life transitions
- Personal stories of kids leaving home
- Research on life-stages and happiness
- What real fatherhood looks like
and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centers’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
Is therapy needed? Tools to try now. (and what is gained from symptoms?)
The latest episode of the Insights & Actions podcast is now available! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD pose the question “Is therapy what’s needed for you now?”
Expect to hear:
- When therapy might not be needed
- Powerful tools you can use now
- Therapy and dating
- Powerful questions to ask yourself to shift your perspective
… and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
If you would like a free consultation with a free consultation with a therapist at Insight Into Action Therapy, contact us: 703-646-7664
Are you at war with yourself? Overcoming your childhood, projection, and taking back your life
The latest episode of the Insights & Actions podcast is now available! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD discuss issues related to personal responsibility, breaking patterns that developed in childhood, and the problem with coping skills.
Expect to hear:
- Personal stories
- How we project and blame others
- Stoicism and buddhism
- Allowing kids to fail
- Courage
…and much more!
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible. Click the links below to watch and listen!
If you would like a free consultation with a free consultation with a therapist at Insight Into Action Therapy, contact us: 703-646-7664
Lawyer Meets Therapists: Personal Stories of Mental Health and the Criminal Justice System
The latest episode of the Insights & Actions podcast is now available! We sit down with defense attorney Jeff Mangino for a powerful, real-world conversation about the intersection of mental health, therapy, and the criminal justice system.
Jeff opens up about his personal experiences with therapy, how life events like divorce and family struggles shaped his perspective, and why he believes therapy is crucial — not just for his clients, but for himself.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible. Click the icons below to watch and listen!
Can I Keep Drinking? Alcohol Moderation Expert Cyndi Turner
The latest episode of the Insights & Actions podcast is now available! Insight Into Action Therapy co-founder and alcohol moderation expert Cyndi Turner, LCSW, LSATP, MAC talks about the controversial topic of alcohol moderation. Ready to move past the binary of “alcoholic” or “not alcoholic?”
In this episode, expect to learn:
- How alcohol moderation works
- How to determine if you are a good candidate for alcohol moderation
- How research into alcohol moderation was suppressed
- Common myths about alcohol moderation
…and much more!
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible. Click the icons below to watch and listen!
Take the alcohol moderation assessment.
Purchase Cyndi’s books (click the book below to purchase on Amazon!)
Psychology “Buzzwords” – Mindfulness, Neurodiversity, and Safety
The latest episode of the Insights & Actions podcast is now available! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD, explore popular buzzwords in psychology—safety, neurodiversity, and mindfulness. Where did these terms originate? How are they used today? And what impact do they have on their field and culture?
This episode covers:
- The roots of mindfulness in Buddhism and its role in modern psychology
- How the pursuit of safety can fuel anxiety
- Different takes on the concept of neurodiversity
- Personal stories and insights
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible. Click the icons below to watch and listen!
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD pose the question “Is college worth it?” They talk about ‘the college obsession’, how parents’ best intentions can go wrong, mental health, and stoic practices for wellbeing.
Also, in this episode
- Statistics on the financial return on investment for going to college
- How do you define success (for your kid)?
- Kids not being allowed to fail
- Input from a school counselor
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD talk about the history and misuse of psychology “buzzwords” in social media and pop culture. They also reflect on a powerful verse from the Tao Te Ching.
The guys discuss:
- Narcissism
- Life Coaches
- Bipolar
- Gaslighting
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
In this clip from the Insights & Actions podcast, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD watch and react to a powerful therapy scene from The Sopranos. In the scene, Tony Soprano and Dr. Melfi discuss his son A.J.’s suicidal ideation, Tony’s guilt, and doubts about therapy.
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD talk about positive trends they’re excited about in mental health therapy.
The guys discuss:
- Not diagnosing normal behavior
- Innovations in therapy
- Psychedelics and SSRI’s
- Using brain scans clinically
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD talk about negative trends they’re seeing in mental health therapy.
The guys discuss:
- Excessive boundaries
- Reinforcing clients to “point the finger at others”
- Creating an identity out of pain
- How some treatment programs take advantage of clients
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD talk about masculinity and vulnerability, male violence and bullying, men’s mental health, and relationships.
In addition, the guys discuss:
- Male violence and bullying,
- Men’s “compartmentalization”,
- The challenges facing different generations of men,
- Self-care strategies,
…and much more!
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
In this clip, taken from the inaugural episode of the Insights & Actions podcast, “The Problem of Overindulged Kids,” Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD discuss whether, as a culture, we are overusing the idea of “trauma.” Furthermore, can therapists become part of the problem?
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
The latest episode of the Insights & Actions podcast is out now! In this episode, Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PsyD explore how therapy can lead to change.
In addition, the guys discuss:
- Does the “type” of therapy (e.g. CBT, DBT, EFT) matter?
- What do mental health diagnoses mean and are they important?
- What led to change in their lives personally
- Will AI therapists become the norm?
- Answer audience question
Have you ever wanted to hear what therapists really talk about when they’re out of session? The Insights & Actions podcast allows you to do just that. Insights & Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
Insights & Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
Have you ever wanted to hear what therapists really talk about when they’re out of session? The new podcast Insights and Actions allows you to do just that. Insights and Actions are candid conversations with Insight Into Action Therapy and Insight Recovery Centerss’ clinical team.
The first episode, out now, is “The Problem of Overindulged Kids” featuring Craig James, LCSW, LSATP, MAC, Matt Christian, LCSW, and Johnny Pierce, PhD.
Overindulgence can take the form of too much stuff, soft structure, and over-nurturing. Though often with the best intentions, overindulgence can contribute to a lack of resilience and confidence, increased anxiety, and eventually failure to launch. Identifying these behaviors is important. However, real change can happen when we move beyond the “what?” to the “why?” Hear Craig, Matt, and Johnny discuss how they see this play out with families in the therapy office, the underlying reasons many parents may be overindulging their kids, and how to begin to make changes.
Insights and Actions can be found on YouTube, Spotify, Apple podcasts, Amazon music, and Audible.
By Matt Christian, LCSW
Grounding Exercise:
We all experience times in which we feel stressed, overwhelmed, checked-out or just “off.” Fortunately, there are techniques to help restore balance. Mindfulness techniques can help relax your body and mind and bring you back to the present moment. Follow along with this guided grounding exercise and come back to it whenever you need to pause and recenter yourself!
Mindfulness Meditation:
Using guided meditations can be very helpful, especially when first exploring mindfulness meditation. Regular mindfulness meditation has been shown to help improve focus and memory, assist in reducing anxiety and depression, and manage physical pain. Studies of meditators have shown changes in areas of the brain associated with emotion regulation and self-awareness.
This short, guided meditation can be a great entry point as it utilizes multiple senses to help us rest our awareness in the present moment.
Thought Defusion:
Have you noticed how racing or intrusive thoughts can lead to suffering? One reason for this is that we become “fused” with our thoughts. This means that we can’t separate ourselves from our thoughts. We get stuck in our head, and the thoughts become our reality. Thought defusion is an important technique in Dialectical Behavioral Therapy (DBT) and Acceptance and Commitment Therapy (ACT). It helps us develop the ability to take a step back and observe our thoughts without getting caught in them.
This guided thought defusion exercise uses guided imagery to help us step back and become “unstuck” from the thoughts that bother us.
If you or a loved one is having a difficult time or would like to explore practices to develop a greater sense of wellbeing, please reach out! Our clinicians at Insight Into Action Therapy are here to provide these tools and many others.
The stigma around mental health and engaging in therapy has often acted as a barrier for people seeking services. In this Insight Minute video, Dr. Johnny Pierce challenges this stigma by proposing a new perspective on mental health care, shifting our focus from illness to wellness.
In the companion “Holding Space” video, Dr. Pierce has a conversation with his colleague Matt Christian, LCSW, exploring the root of this stigma and showing why in the end, the stigma just doesn’t make sense.
If you or your loved one is experiencing mental health difficulties and would like to embark on the journey towards wellness, please reach out to our team at Insight Into Action Therapy!
In my almost 30-years of working in the addiction treatment field, the most common question clients ask me is “can I keep drinking?” I have found that there is over 50 years of research that shows that many people actually can.
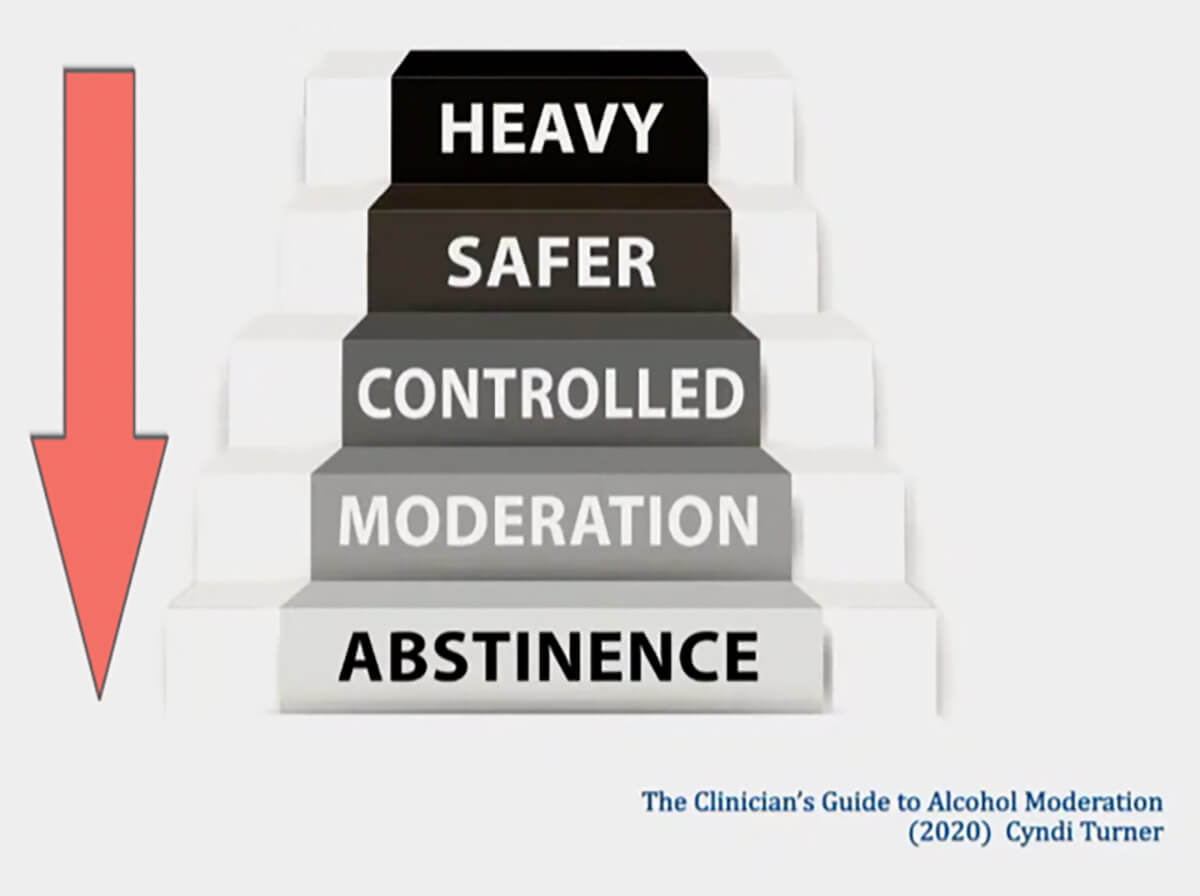
In our culture, and even in the substance use treatment field, people often view problems with alcohol as a binary, either you’re an “alcoholic” or you’re not. The reality is that there is a spectrum of alcohol use. The image that many have of an “alcoholic” – physical dependency, withdrawals, severe consequences – only account for around 6% of people that occupy the far end of this spectrum. For these people, long-term sobriety may indeed be the safest option.
However, there are many people who are aware that they have a problematic relationship with alcohol but for whom complete abstinence is a non-starter. Unfortunately, when they seek help, they are told that they must pursue long-term sobriety. These people typically drop out of treatment and never receive the tools they need to develop a healthier relationship with alcohol.
So, how might someone determine if they are a good candidate to try alcohol moderation? I developed the Alcohol Moderation Assessment to help answer this very question. Furthermore, I’ve made this tool available to the public.
The 20-question assessment consists of research-based predictors, both positive and negative, that can help one gain insight into whether they may be a good candidate to drink in moderation. Upon completion of the assessment, a score is given that corresponds to the likelihood that one will be able to successfully practice alcohol moderation.
If you are interested in pursuing alcohol moderation, there are resources available to help you on that journey. I have published a workbook titled “Practicing Alcohol Moderation – A Comprehensive Guide” that provides practical strategies for implementing alcohol moderation. One can also check out the mutual support group Moderation Management or work with a clinician trained in alcohol moderation.
If you or a loved one are struggling with alcohol use, Insight Into Action Therapy is here to help you on your journey towards developing a healthier relationship with alcohol.
When most people think of substance use treatment, they think “rehab.” Specifically, 28-day inpatient rehabilitation programs. This is when I like to pause and ask questions: “Why 28 days?”, “What is someone trying to achieve by entering a 28-day rehab program?”, “Is this the best form of care to meet their needs?”
The truth is, “28-day rehab” is not a medical model. Rather, it was originally a military model. For example: a soldier at Fort Bragg is out of control with their drinking and has one month before reassignment to Fort Belvoir. They may be told, “take these 28-days and get yourself together.” This wasn’t designed by clinicians as an ideal therapeutic model.
In fact, I don’t call inpatient rehab treatment, I call it stabilization. While an individual with a severe substance use disorder may need detox and even an inpatient program, 28 days usually isn’t enough. In practice, it may look something like this: Week one, they’re detoxing. Week two, they’re upset that they’re there. Week three, they may be starting to “get it,” and by week three-and-half to four they’re getting ready for discharge. It just isn’t enough time. They often return to the same environment in which their substance use was occurring and are at high risk for relapse. Moreover, I often see family members spend tens of thousands of dollars as their loved one cycles in and out of rehab facilities.
So, what might a better model look like? Broadly speaking, a more comprehensive approach is needed. If an inpatient rehabilitation program is necessary, it’s important to be realistic about what it can achieve. I believe it should be viewed as an initial step. It can provide enough clean time that one can then more successfully engage in treatment in the community. This treatment may include an intensive outpatient program, individual and family therapy to address mental health difficulties, medications if necessary, repairing relationships, and assistance in obtaining employment and housing. Many also find it helpful to participate in mutual support groups, such as Alcoholics Anonymous.
When speaking with family members whose loved one is in an inpatient rehabilitation facility, I always ask: “What’s the plan for when they are discharged?” I really empathize with individuals and families who are struggling with substance use. It’s stressful and confusing to navigate the different treatment options. Here at Insight Into Action Therapy, we specialize in developing individualized treatment plans that honor everyone’s unique needs. If you or a loved one is struggling with substance use, we’re here to help.
In my work as a therapist, I frequently utilize mindfulness practices with clients. Mindfulness is an important feature of many of the newer approaches to therapy that build on the techniques of Cognitive Behavioral Therapy (CBT) — often cited as a preferred form of therapy, given the extensive research on its effectiveness.

Clients having difficulty with anxiety and depression often describe their mind “spinning out” with worries or negative thoughts about themselves or the future. By gaining greater ability to bring our attention to the present moment, we can stop fighting with our thoughts and find more peace.
However, at times I wonder if there is something missing in this “medical” way of presenting mindfulness. It may be because before training as a therapist, I was training in meditation traditions that mindfulness practices come from. In short, my uneasiness is this:
Just becoming a little more peaceful wasn’t the original purpose of mindfulness. Rather, these practices were designed to facilitate important insights that can decrease our suffering in a more fundamental way. Specifically, insights into things such as:
- the moment-by-moment impermanence of all things,
- how craving and “clinging” lead to suffering, and
- the very nature of the self, or “ego.”
Importantly, these insights are experiential, not just intellectual. As an analogy, we can get some understanding of the beauty of love by reading philosophy or poetry. However, it’s the experience of love — maybe the love for a spouse or a child — that can transform our lives. Similarly, it’s the experience of clearly seeing how our mind creates suffering that provides the potential for greater change.
As I mentioned at the beginning of this blog post, I’m a big proponent of using mindfulness in therapy. However, if working with mindfulness really resonates with a client, it may be important to let them know that these practices have the potential to go much deeper should they feel called to pursue it outside of therapy.
If you or someone you love is struggling with their mental health or substance use, Insight can help. Please call 703-646-7664 for more information
Matt Christian, LCSW
Though more people are becoming familiar with the term “dual diagnosis”, let’s first get clear on what it means. Simply put, it’s when an individual has both a mental health disorder and substance use disorder simultaneously. This is not a rare occurrence. In fact, it is estimated that around 50% of people with a substance use disorder have a cooccurring mental health disorder. As a clinician, I’m always screening for both during the assessment process.
So, why is this important? Untreated mental illness leads to higher rates of relapse and worse outcomes overall. Nothing in our lives exists in a vacuum. Treatment that focuses on just substance use or mental health is less effective. It’s all about integrated care, in which both are addressed simultaneously. We need to be treating the whole person.
In practice, integrated care can take many forms and needs to be tailored to the individual. Some potential features of integrated care may include:
- Individual and/or group therapy,
- Meeting with a psychiatrist for medication to treat the mental health disorder, or medications that reduce cravings for substances,
- Involving important stakeholders (e.g. parents, spouses, support networks),
- Helping the client seek and maintain employment,
- Strategies for building healthy relationships, and
- Referrals for higher levels of care when needed.
In my view, a crucial element of integrative care is to have a clients’ providers communicating and collaborating on the case. Unfortunately, in my experience, it can often be hard to get responses from psychiatrists and other providers. This is understandable as oftentimes they have very large caseloads that don’t allow for frequent, in-depth conversations with a client’s therapist.
A luxury that we have at our practice is that we have psychiatrists “in-house” that I have frequent contact and personal relationships with. When I have a client who is also seeing one of our psychiatrists, it is easy for us to call the other or talk about cases when there is downtime in the office. Regardless, it is often important for clients and their loved ones to build a treatment team that is experienced in working with dual diagnosis.
While these cases can be complex, I have confidence in people’s resiliency and ability to heal. It’s never a straight line of progress; there will be ups and downs along the way. However, a healthier, more fulfilling life is possible. People who are struggling aren’t just a “diagnosis” or defined by their difficulties. They have great strengths that help them on their journey towards wellbeing. As a clinician, being a part of that journey is a great honor and joy.
If you or someone you love is struggling with their mental health and substance use, we can help. Please call 703-646-7664 for more information.
When working with clients on their substance use, there’s one tool I always use. Though it seems simple, it can be powerful and lead to insights. It’s a Cost/Benefit Analysis.
Cost/Benefit Analysis:
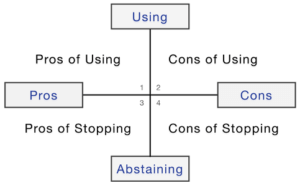
Clients are surprised when I tell them to put a big “X” in quadrants 2 and 3. I don’t care about these areas. People typically know the consequences if they use. It’s logical. Quadrants 1 and 4 is where the therapy happens. Working with these quadrants gets to their “why?”.For us it’s always the “why?” We must get clear on why they began using in the first place and what they get from their continued use.
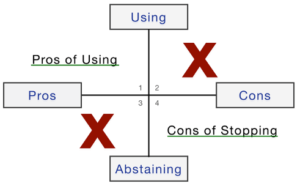
Particularly quadrant 4: What are the downsides of stopping your use? What would your life be like without the substances? What would you have to deal with? This gets to the “why?”. Only focusing on behavior without addressing the “why?”, often lacks the power to lead to lasting change.
While the substance use is having a negative impact overall, taking the substances away is a real loss. Strategies to help replace the benefits of using and working with underlying issues is what’s needed. By taking clients through this activity, I’m trying to push beyond their behavior – I’m trying to get to their “why?”
By the time clients come to see me, their substance use has often been damaging their lives for some time. As they begin taking steps to achieve sobriety, I always honor that losing the substances can be a real loss. There’s something that they were getting from the substances, especially at first. It may have been working for them for a time. So, when something so central to their lives is being taken away, something must be put in its place. Just stopping the use isn’t enough. The goal is to be living a fulfilling life, not sobriety for sobriety’s sake. Any change to their substance use needs to be in service of that goal.
When beginning to work with clients who are newly sober, I start by helping them develop practical, present-focused strategies to manage their distress. It’s about working with all areas of their life and building positive momentum. For example, when their anxiety becomes more manageable, it then becomes easier to make other changes. That could include obtaining employment or improving their relationships. As they begin to feel more connected and see their life improving, they may feel more motivated and confident to keep going. In practice, this is never a straight line of progress in which things get better and better each day. The process can be messy. There will be setbacks. But every positive step is planting a seed for further change.
By acknowledging that removing substances can feel like a genuine loss, the therapeutic process becomes more collaborative. It reinforces that they are not being judged for their substance use and that they have a partner in their journey of building happier, healthier life.
The substance use treatment field is the only one I know of in which if you show signs of a problem, they kick you out. Someone goes into a treatment center, is found to be using substances, and then is discharged. Let’s step back and considered the logic of this… Someone goes into treatment for a problem, is showing symptoms of that very problem, and then is kicked out as a result. My response is: “If I had heart disease would you kick me out of care if my blood pressure was too high?”
Most clinicians are looking for an outcome, usually abstinence. In my view, while the goal may be abstinence, we’re trying to reduce the harms of drugs and alcohol to get down to a healthier level. An over-focus on a specific outcome (abstinence) can get in the way of effective treatment. It is not realistic regarding what the journey of recovery entails. It doesn’t honor that these clients are at high risk, and that harm reduction is needed to give clients an opportunity to discover greater wellbeing. So, why do some providers kick people out of treatment? Because they’re uncomfortable with this process. I often say, “I don’t care about the outcome. I like the process.”
Part 2: Observations from the therapy office
In my last video and blog post, I discussed why the pandemic might be affecting teens’ mental health in unique ways. Here, I’d like to share some observations from working with teens’ during the pandemic – from the days of scrubbing groceries with Clorox wipes, to googling: “how do you pronounce omicron?’”. What follows are some trends I’ve noticed, and of course do not represent the full scope of teens’ experience during the pandemic.
I’ll refer to these trends as:
- “The great malaise” (“this doesn’t feel real…”)
- “The social anxiety swing”, and
- A Rise in Self-harm
The great malaise:
As unbelievable as it now seems, in the early days of the pandemic we believed that the lockdowns, school closures, and social distancing would be short-lived sacrifices. However, there came a point when we collectively acknowledged, “oh, this isn’t going away any time soon.”
For many of my teen clients, the transition from the pandemic being a departure from normal, to being the new normal, triggered a downward slide. Many began presenting with depression-like symptoms. They reported having less energy, their sleep schedules became erratic and things that they typically enjoyed became less interesting. There was a general undercurrent of helplessness.
And then there was school. Many once high-achieving students began to feel less and less motivated. I often was told “it (school) doesn’t feel real.” The virtual learning wasn’t working for them. The routine became wake up, log-on, turn off the camera and microphone, and go back to sleep or play video games.
Many of these clients weren’t technically in a major depressive episode (though I did see a significant uptick in teens presenting with a major depressive disorder during this time). Rather, what I observed was a pervasive fog of low-level depression amongst teens.
The social anxiety swing:
For my teen clients with social anxiety, the pandemic initially led to relief from their symptoms. The reason was obvious: lockdowns and social distancing removed the triggers of the anxiety. More than that, they were being required to not interact with others. So, there wasn’t the uncomfortable push from parents (or their therapist) to continue doing the anxiety-provoking work of exposing themselves to social situations.
Why do I call this the social anxiety swing? Well, as restrictions lifted and they began in-person school and activities, their social anxiety was more intense than when the pandemic began. This is also not surprising given how anxiety often works. If something triggers anxiety, it is avoided, leading to temporary relief. However, as one gets stuck in these anxiety/avoidance loops, that same trigger brings on more intense anxiety over time. Additionally, two years of significant isolation during adolescence can stunt the development of social skills, which can also contribute to social anxiety.
Rise in self-harm:
A rise in suicide attempts during the pandemic, particularly among young girls, has rightfully received a lot of attention. Indeed, the surgeon general report states:
In early 2021, emergency department visits in the United States for suspected suicide attempts were 51% higher for adolescent girls and 4% higher for adolescent boys compared to the same time period in early 2019.
However, the form of self-harm I’m discussing is different. I’m referring to my teen clients cutting, burning, hitting, or scratching of themselves as a coping mechanism. Typically to help deal with intense, out of control feelings, or conversely, if they’re unable to feel anything at all.
I had many parents bring their teenage kids in after discovering they were self-harming. In most of these cases there was no prior history of self-harm. Now,the causes for any particular client are typically complex. However, a common theme expressed to me was that they felt that their and their family’s lives, and the world itself, was out of control. A feeling I believe we can all empathize with.
I hope this helps give a feel for the struggles many adolescents experienced during this pandemic. If you or your teen is having a hard time, you’re not alone. Please reach out for help!
If you would like a free consultation with a therapist at Insight Into Action Therapy, please contact us!





